When I started training as a psychiatric nurse in the late 1980s, we had a class on death in the initial module before we were let loose on unsupecting wards, and I was surprised by how many people had to take advantage of prior permission to step outside for a while should one feel the need.
Later on, we were introduced to psychiatric nursing proper, and we all did the training; those were the days when heads of nursing schools were more involved in working with hospitals than now, and it was realised that sometimes people with mental illnesses or learning difficulties need to come to hospital, or conversely staff in mental-health institutions might need general-nursing skills should one of their charges, say, become ill or have an accident.
In this module, we were introduced to suicide as a subject for clinical study, and everybody was expected to stay within the lecture hall: everybody did.
First came an anecdote of a man who said every day that he was going to kill himself, how, and where: and one day, after several years, as people paid less and less notice, he did. The moral: never take a threat or prediction of suicide anything other than seriously. On the other hand, there were also people who would be admitted having injured themselves in ways which self-evidently c
 ould not be life-threatening - but navigating around the large intersect between the two approaches the best definition of psychiatry I've ever heard: "a blind man in a dark room looking for a black cat that isn't there".
ould not be life-threatening - but navigating around the large intersect between the two approaches the best definition of psychiatry I've ever heard: "a blind man in a dark room looking for a black cat that isn't there".Over the years I lost several clients to suicide, which was quite hard at the time. But then I lost a friend, and experienced first-hand the raw nerves slicing across one's consciousness as emotional evisceration accompanies an endless round of "what-ifs". I still ask the girls to help me pray for "Dad's friend who died sad and alone", and I think Minora's guessed what that means.
So my antennae twitched upon reading a story on the matter in the Cambridge News.
In December 2006, 56-year-old David Woods was admitted to Addenbro
 oke's Hospital in Cambridge after a suicide attempt. His daughter and son were alerted. By the time they arrived in Cambridge, Mr Woods had been given a liver transplant as an urgent life-saving measure. Neither of his children had been consulted.
oke's Hospital in Cambridge after a suicide attempt. His daughter and son were alerted. By the time they arrived in Cambridge, Mr Woods had been given a liver transplant as an urgent life-saving measure. Neither of his children had been consulted.Mr Woods was in a coma for six weeks after the incident (it's not mentioned whether it was medically induced), and came to with, we are told, "the mental age of a child" who needs round the clock care. So, given that the attempt that landed Mr Woods in hospital came at the end of a rapid succession of tries that day, why was a liver transplanted; and why is this three-year-old incident hitting the news big-time now?
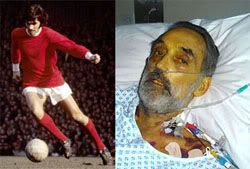
Looking at the first question yields clouds within clouds. Professor Roger Williams of University College's Institute of Hepatology in London was involved in Great Britain's first liver transplant in 1968, and was also involved in the care of George Best towards the end of his life, imploring every pub and off-licence in the country not to serve alcohol to the addicted footballer. He told the Telegraph's Celia Walden:
"What is surprising is that the family do not appear to have been consulted," he tells me. "When we first started conducting liver transplants in paracetamol overdose cases, most were young people without a history of psychiatric illness. Very few would be given a transplant within 24 hours without agreement from the family...I find it puzzling that these things weren't picked up on when the clinician reviewed David Woods' notes. It is very unusual for someone to be given a transplant when they have tried to commit suicide several times in the past.Williams was speaking about the effect this affair might have on potential liver-don
 ors; but I do't think I would be straying from the pro-life fold by suggesting that a liver transplant, with the attendant risk of major damage to organs - including the brain - through buildup of toxins should not be undertaken until the family's view has been taken into account. I'm not saying for a minute that anybody who is critically ill following a suicide attempt shouldn't be treated, merely that in this particular instance a unilateral decision to insert a donor liver may have been something of an unreasonably heroic measure.
ors; but I do't think I would be straying from the pro-life fold by suggesting that a liver transplant, with the attendant risk of major damage to organs - including the brain - through buildup of toxins should not be undertaken until the family's view has been taken into account. I'm not saying for a minute that anybody who is critically ill following a suicide attempt shouldn't be treated, merely that in this particular instance a unilateral decision to insert a donor liver may have been something of an unreasonably heroic measure.Professor Williams adds: "I would say that the psychiatric assessor is the person one might point a finger at"; it's not clear that the psychiatrist who examined David Woods while he was semi-conscious at best was employed by Addenbrooke's or the local mental health trust, but it would be instructive to look at the latter, who would have treated him for his manic-depression.
In November 2006, the Cambridgeshire and Peterborough NHS Foundation Trust's board meeting minutes announced that "performance targets" for its annual health check by the Healthcare Commission (now the Care Quality Commission) included an "Audit of suicide prevention". This was a month before Woods' last attempt, but five months after an earler attempt, we are told, was assessed as a "cry for help". (The suicide prevention audit is first mentioned in board minutes of March 2006.) In March 2008's minutes we learn that the annual healthcheck has been passed except for a waste-management target, and "A re-audit of the National Suicide Strategy in 2007 identified clear improvements in clinical practice" and that "
the electronic system for investigating and completing serious untoward incidents (SUIs), was reviewed and further improved during the year and now incorporates the national standards for suicide prevention."
An annual healthcheck is a byzantine proceedure looking at a trust's "performance indicators"; in the "frequently asked questions" document, on page 12 (of 15), we learn in the answers to questions 24 and 25 that "It is the responsibility of every healthcare organisation to ensure that they submit all necessary data for our assessment purposes by the deadline date for each data collection...It is the responsibility of the primary data collector to communicate these data quality checks and ensure that they are applied prior to submission to the Care Quality Commission."
So there we have
 it: two levels of deniability between the Care Quality Commission's examining whether boxes are ticked and conditions endured by patients (and staff) on the ground. It comes as no surprise that the Care Quality Commission is headed by Cynthia Bower, former chief executive of the West Midlands Strategic Health Authority when it failed to pick up the egregious abuses visited upon patients in Stafford General Hospital. She wouldn't have been in place at the time we're talking about, but she has obviously been parachuted into a job where her talents will ensure the continuation of the prevailing ethos.
it: two levels of deniability between the Care Quality Commission's examining whether boxes are ticked and conditions endured by patients (and staff) on the ground. It comes as no surprise that the Care Quality Commission is headed by Cynthia Bower, former chief executive of the West Midlands Strategic Health Authority when it failed to pick up the egregious abuses visited upon patients in Stafford General Hospital. She wouldn't have been in place at the time we're talking about, but she has obviously been parachuted into a job where her talents will ensure the continuation of the prevailing ethos.Cambridgeshire and Peterborough NHS Foundation Trust's medical director, Dr Tom Denning, told the Cambridge News in the article linked to above that "you always have to give life the benefit of the doubt". The Trust has just published a statement on the "latest news" section of its website:
We are sorry to hear that the family have concerns about whether in retrospect it was the right thing to undertake a life saving liver transplant operation in 2006. We would like to hear from the family so that we can discuss their concerns in more detail.Personally, I think this bit of get-outery is of doubtful value, and I would suggest that David Woods was given a liver transplant - whatever the result - without reference to the family in order to improve Cambridgeshire and Peterborough NHS Foundation Trust's appearance of compliance with suicide-prevention targets.
Decisions to undertake emergency life-saving liver transplantation are made by the transplant consultants with advice from other medical specialists, including psychiatrists, when appropriate.
You'll be glad to know that the answer to the question of why this is an item now is much simpler. But I should first note that I am not implying that David Woods' children have any sort of double agenda. To paraphrase a wise family doctor's counsel to my wife when I was first diagnosed with manic depression, they've been hit by the train, and it keeps on hitting.
On 27 May, the story broke in the Cambridge News and it was mentioned that Nadine Woods was "torn" about taking her father "to a euthanasia clinic in Switzerland".
The next day (the same day that the Telegraph picked up the story), Lord Alderdice tabled an amendment to the Coroners and Justice Bill, which is due to be debated in a House of Lords Committee on 9-10 June. The amendment reads:
Insert the following new Clause—Although SPUC director John Smeaton states the amendment is not likely to be added to the bill, it's important that it be opposed vigorously to show that people who value life are alert to the drip-drip-drip of bringing legalised euthanasia onto the statute books against the will of the British people - and the Members of the House of Lords might want to look in the direction of the Commons to see the effects of continually acting against the interests of the people one is supposed to serve.
"Exceptions to offence of assisting suicide"
Notwithstanding sections 49 to 51, no offence shall have been committed if assistance is given to a person to commit suicide who is suffering from a confirmed, incurable and disabling illness which prevents him from carrying through his own wish to bring his life to a close, if the person has received certification from a coroner who has investigated the circumstances, and satisfied himself that it is indeed the free and settled wish of the person that he brings his life to a close."
If you live in Great Britain, please read and act upon this alert from the Society for the Protection of Unborn Children. If you from elsewhere, please pray for us.
And for the Woods family, who find themselves buffeted by agendas more highly-powered than most express trains.
Depression's a queer thing to deal with - everybody has their own way to deal with the Black Dog, as Churchill called it. There's always the Samaritans, of course, or a doctor, friend, counsellor, or the local mental health helpline. Myself, if I'm too down to read a book, I turn on the radio, preferably a station with some MOR music and light banter. The mood-lifting effects of exercise have long been noted, but if I embark on some hard-training plan I end up beating up on myself when, inevitably, I fail: walking is good. REM has some good advice in their song Everybody Hurts - "take comfort in your friends". I find it incredibly difficult to tell people face-to-face when I'm down, but I hae to because I hide it when I am; and my friends give me time when I manage to tell them, whether that be time spent with me or time I need to take to reforge connections after a period not really saying much. And as a very wise man I knew once said, if the abyss looks into you when you look into it, look the other way.












No comments:
Post a Comment
Please feel free to leave a comment - Frugal Dougal.